|
By Dr. Annesha Foote
Mosquito borne diseases have been a hot topic for the past few years since the rapid spread of Chikungunya through our country followed by Zika, and the yellow fever outbreak in some countries. Humans have not been the only ones afflicted by these annoying pests, our dogs and cats have also been afflicted. Long before any of the other diseases made their presence felt on our shores, heartworm has been a nuisance for many of our pets.
READ MORE
|
| Paraquat (Gramoxone) Poisoning in Dogs |
| Better known as Gramoxone, Paraquat is a commonly used and readily available herbicide in Jamaica. It is also one of, if not the most common poisonings that occur in dogs. Unless ingestion is detected and dealt with almost innediately, it is almost invariably lethal, often causing a slow and agonizing death.
Humans have used it to commit suicide and there is evidence that exposure may lead to Parkinson's Disease, yet it remains readily available in Jamaica's farm stores despite the fact that its use is heavily restricted or banned in much of the developed world. It's popularity as a herbicide stems from its effectiveness in that role, low cost and its quick decomposition when it interacts with soil.
Paraquat's toxic effects occur in the kidneys, liver and, most prominently, in the lungs. Very high doses result in severe, acute kidney failure which can cause death within a few days. With lower doses, the predominant sign in dogs is deep and laboured breathing, groaning, cyanosis (gums turn purple due to lack of oxygen in the blood) and gradual suffocation. The chemical induces a free radical reaction in the lungs causing destruction of the lung tissue and, if the animal survives the initial insult, scarring of the lungs (fibrosis) restricting their ability to expand. Even a small dose can set off the reaction, which self-propagates, leading ultimately to death. The very oxygen in the air that is necessary for life becomes part of the free radical reaction.
Treatment is generally unrewarding, unless started extremely early. Early treatment is unlikely as many dog owners only notice there is a problem is when the animal begins laboured breathing - at that point it is generally too late. It involves using anti-oxidants to control the free radical reaction, duiretics to flush the chemical from the system, and adsorbents to reduce absorption from the intestinal tract, along with other supportive measures.
There is a test available to confirm a diagnosis of paraquat poisoning.
To prevent exposure, do not use Gramoxone/Paraquat on your premises if you have pets, Do not allow dogs to roam outside of your premises. If you are capable of or have access to advanced dog training techniques, train your dogs not to eat anything other than the food you provide for them.
For more information on Paraquat see the following:
Click HERE for Prof. Cecil Brownie's infosheet on pesticides and herbicides. Scroll to Page 54-56 for Paraquat.
Click HERE for a detailed DVM-360 Article "Toxicology Brief: Helping animals exposed to the herbicide Paraquat".
|
| FELINE DIROFILARIASIS - Heartworm in Cats |
 |
| Photo courtesy of Dr. Robert Wan |
|
| The Canine Heartworm, Dirofilaria immitis, is a nematode worm of the super-family Filaroidea, that is known for causing an often debilitating and fatal infestation in dogs. Spread by mosquitoes which deposit infective L3 larvae when they feed, the worms undergo a 6-month migratory development phase at the end of which they emerge as adults in the right ventricle of the heart and the pulmonary artery which carries blood to the lungs.
Adults, which are male and female, produce microfilaria – microscopic “babies” that circulate in the blood and are picked up by feeding mosquitoes to start the cycle again. Depending on the number of adult worms present, the dog may be asymptomatic or may develop progressive illness, with clinical signs such as a chronic cough, weight loss, exercise intolerance, fluid accumulation in the abdomen (ascites) ultimately leading to death.
It is treated using a specific drug, melarsomine, to kill the adults, followed by a long recuperative phase to allow the immune system to break down and eliminate their remains. Prevention is accomplished by the regular use of ivermectin or related drugs to eliminate the developmental stages before the adult stage is reached. Ivermectin is NOT effective against the adults.
But what of cats? Cats are infected with L3 larvae by mosquito bites as well, and these do undergo migration as occurs in dogs. Some may survive long enough to end up in the lungs causing Heartworm-Associated Respiratory Disease (HARD) in which the cat may show a chronic cough, wheezing or difficulty breathing. Others may achieve adulthood, emerging in the heart and pulmonary artery as happens in dogs. Affected cats may show similar clinical signs to dogs, but also may show vomiting and breathing difficulties. In some cases, the only sign is sudden death.
Cats with heartworm disease involving adult worms in the heart cannot be treated with melarsomine. It is fatally toxic to them. At this time, surgical removal of the worms is the main option and is not a simple procedure.
Cats in heartworm-endemic areas therefore need to be kept on monthly ivermectin prevention.
For a report on a case of Feline Heartworm Disease in Jamaica, which includes more details, please click HERE. Thanks to Dr. John Josephs of Noah’s Ark Veterinary Centre.
Heartworm can affect HUMANS too.
For information on Heartworm in HUMANS, please click HERE.
|
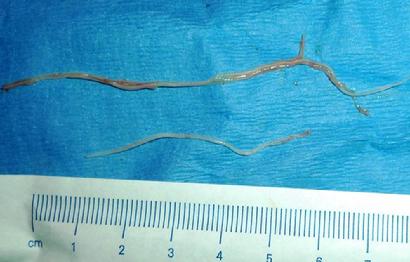 |
| Heartworms removed from the heart of a cat that died suddenly. Photo courtesy of Dr. John Josephs. |
|
|
| CANINE INFLUENZA H3N2 SPREADS IN THE U.S. |
A new strain of Canine Influenza - H3N2 - has been spreading rapidly in the United States Mid-west - with as many as 1,000 cases reported in dogs in the Chicago area. This strain has also reportely affected cats.
H3N2 is an Asian flu strain, distinct from the H3N8 strain that has been circulating in the US since 2004. There is a vaccine for the latter, but it uncertain (and unlikely) that it can offer any protection against the new strain. Diagnostics specific to H3N2 are under development.
The clinical picture and epidemiology for the two strains are similar, as is treatment. There is no evidence of dog to human transmission, although this situation is being monitored.
There is NO evidence of Canine Flu in Jamaica.
Click here for information from the United States Centers for Disease Control & Prevention (CDC)
| |
The Canine Infectious Respiratory Disease (CIRD) Complex, commonly known as “Kennel Cough”, which includes a number of infections such as those caused by Bordetella bronchiseptica, Canine Adenovirus-2, Canine Parainfluenza virus, Canine Distemper Virus, had a new viral disease added in 2005. In the United States, the Equine Influenza virus A-H3N8 made the species jump into dogs– greyhounds in Florida at first in 2004, then to others in other states – becoming Canine Influenza Virus (CIV A-H3N8)2.
Canine Influenza is completely distinct from Canine Parainfluenza which is caused by a different virus, though they have similar effects. It is highly contagious, can affect dogs of all ages and is transmitted by direct contact, aerosol or via contaminated objects – including human hands. Of exposed dogs, 80-90% will develop clinical infection and up to 20% of these develop severe disease, including possible pneumonia from secondary bacterial infection. The disease, like its equine counterpart, is not known to be transmissible to humans3.
Clinical signs include fever, a productive cough, mucoid to mucopurulent nasal discharge, with more severe cases showing lack of appetite, and, if pneumonia develops, more severe respiratory signs such as dyspnea (difficulty breathing). The clinical course may run from 10 to 30 days. Mortality is low ( 1 – 8%) and is of greatest risk in dogs developing complications1,2.
Definitive diagnosis may be achieved via several laboratory methods including serology, virus isolation and polymerase chain reaction (PCR)1. Each has its limitations.
Treatment is generally supportive. Antibiotics may be used to control secondary bacterial infections that may cause pneumonia, but will not affect the viral infection. Oseltamivir (Tamiflu®)may be used in shortening the course of the disease if started early, but this is generally not useful as by the time the disease is distinguished from other CIRD causes – if it is at all – it is too late to make a difference. Other supportive measures might include non-steroidal anti-inflammatories for fever, expectorants to facilitate clearance of mucus from the lower respiratory tract (cough suppressants are contra-indicated), and, if needed, intravenous fluid therapy1,2.
Prevention may be achieved by vaccination1,2,3 (Novibac® Canine Flu H3N8 – Merck Animal Health), but owners of affected dogs are advised to keep them from mixing with others. General hygienic measures such as hand washing after handling dogs, before handling others may be helpful1,2,3.
Canine Influenza has not yet been diagnosed in Jamaica and should not arrive here easily unless an infected dog is illegally imported.
|
 |
| Canine Influenza A-H3N8 is NOT known to occur in Jamaica |
|
|
 |
| The H3N8 Flu virus http://www.h3n8flu.com/wp-content/uploads/2011/06/h3n8.jpg |
|
|
References:
1 - Canine Influenza (Dog Flu): www.doginfluenza.com
2 - The Pet Health Library, Wendy C. Brooks, DVM, DipABVP, Canine Influenza H3N8 http://www.veterinarypartner.com/Content.plx?P=A&A=2165&S=0&EVetID=3001644
3 - U.S. Centers for Disease Control (CDC) Key Facts about Canine Influenza (Dog Flu): http://www.cdc.gov/flu/canine/
For more information on Canine Influenza please click on the appropriate link below:
Link for Health Professionals
Link for the General Public
|
| CANINE DISTEMPER REVISITED |
 |
| Click on the above image for more detailed information on Canine Distempter |
|
| Canine Distemper is an "old" disease that was once diagnosed with a fair frequency. Despite long being superseded by Parvovirus as THE top canine viral disease in our practices, and suppressed by vaccination, Distemper still persists and will be encountered from time to time.
Distemper is a highly contagious, debilitating, multisystemic viral disease of carnivores including dogs, ferrets, raccoons, lions and ocelots. The virus is an RNA Morbillivirus loosely related to the human measles virus and the rinderpest virus of ruminants.
The distribution is worldwide and domestic dogs are considered important reservoirs. The highest incidence of disease is found in young (2-6 months old) unvaccinated dogs. All body secretions and excretions of infected animals are infectious. Transmission is primarily via inhalation of aerosolized body secretions or contact with fomites. Transplacental infection may occur rarely. Recovered animals may shed the canine distemper virus (CDV) for 1-2 weeks post recovery but rarely 60-90 days post recovery.
Clinical signs observed are variable and may be general/non-specific, respiratory, gastrointestinal, ocular and neurological. While no specific therapy exists, treatment is attempted via supportive and symptomatic care.
Prevention is best done through vaccination of young pups from 6 weeks until 16 weeks of age with the CDV modified live virus and yearly boosters for adults.
For details on Canine Distemper, please click on the photograph to the left.
Acknowledgements: Dr. Roxanne Bennett, Dr. Kareen Robinson
|
|